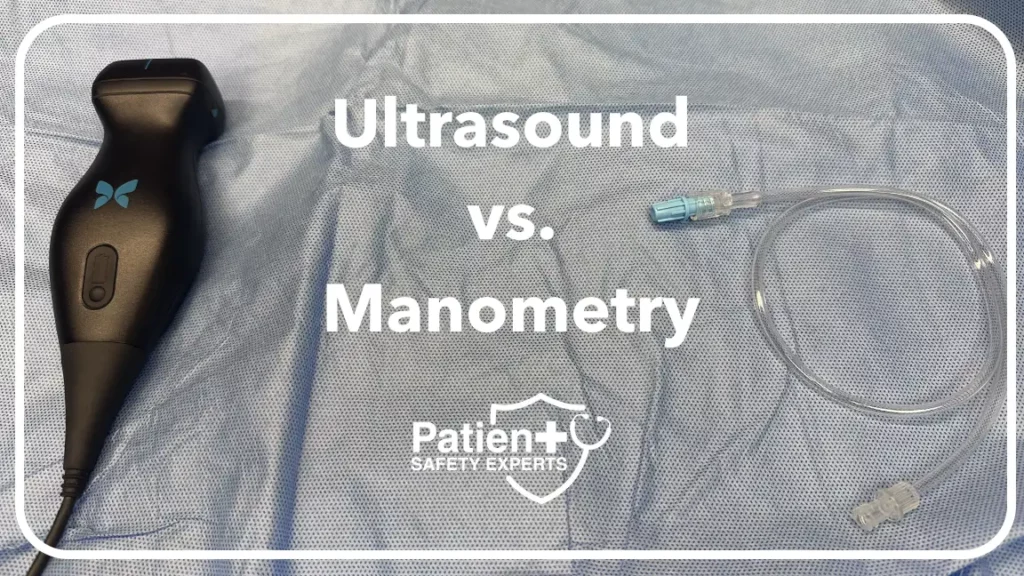
Central venous catheterization is a vital medical procedure, widely used in various healthcare settings. While it plays a crucial role in patient care, it also carries inherent risks, including arterial puncture, pneumothorax, and infection. To mitigate these risks and ensure patient safety, two primary techniques are commonly employed: manometry vs. ultrasound. In this comprehensive comparison, we will delve into the benefits and drawbacks of both methods
Ultrasound vs. Manometry Overview
Central line placement is a very safe procedure in experienced hands. However, each year a new group of medical trainees arrives and needs to be quickly educated about how to perform safe central line placement. If you are a trainee looking to learn safe central line placement, there are two key techniques for safe central line placement: Ultrasound use and manometry.
One common source of confusion and debate between many instructors during central line placement is: if we are using ultrasound do we still need manometry?
Before we get any further into the topic the debate is simple: use both!
Ultrasound and manometry each provide a different type of information which is used together to confirm that the tip of your needle or catheter ( see our article, Central Placement: Steel needle vs angiocatheter ) is in a vein and not an artery before you proceed to dilate the vessel.
The Benefits of Using Ultrasound for Central Line Placement
I am an ultrasound fan. I use the ultrasound for most procedures that I perform as an anesthesiologist. Not because I lack the skills to perform procedures without an ultrasound but because the ultrasound makes me more reliable for everyone around me, especially the patient.
First: Ultrasound helps shorten the time to access the vessel.
First and foremost, ultrasound use does not add meaningful time to the average procedure if you have a system that has the ultrasound available without waiting. If you wait to use the ultrasound only when it’s difficult, there will be delays involved, thus I prefer having to tools I need available from the beginning.
I trained during the landmark technique era when almost every central line was placed using the landmark technique with a finder needle.
When the patient’s anatomy is normal and the operator is experienced, the landmark technique will win the speed contest hands down! I will not argue that. Thankfully we have moved on from a speed-at-all-costs era in healthcare and are focusing more on outcomes for the patient.
Ultrasound shortens the procedure time by:
- Reducing the number of outliers from your central line placement average.
- Allows for pre-scanning of the vessels when considering line placement and allows for proper site selection.
- Allows for troubleshooting wire placement if difficulties are encountered
Second: Ultrasound allows for confirmation of the wire position and troubleshooting
Once you have accessed the vessel, it is crucial to confirm that you are placing your wire into the correct vessel. With ultrasound, we can visualize the wire in the correct vessel.
This process is not bulletproof, however. There are case reports such as these that report the wire going through the vein and into the artery.
Real-time manometry with the Compass Device
While we still perform manometry using a 30cm length of IV tubing, there are newer devices on the market such as the Compass device by Centurion which provides real-time digital pressure reading of the needle tip.
I don’t have any relationship with the device or company but if you want to learn more, here is the website: Centurion Compass
The combination of this device with the Arrow Raulerson Spring-Wire introduction syringe allows for manometry and wire placement without having to detach or remove any syringes or devices.
Safety is the number one priority. Do no harm.
Injury during a central line placement can result in a claim payout, on average, of $95,000 excluding legal expenses. (1 )
Real-Time Manometry with IV extension tubing:
The most common way to perform manometry is to use IV extension tubing to create a column of blood the same way you would measure a CVP.
After you access the vessel, you attach your IV extension tubing to the hub of your needle or catheter depending on which technique you are using to obtain venous access.
To learn more see: Central Line Placement: Steel Needle vs Angiocatheter.
The Role of Various Specialties in Central Line Insertions:
Who is placing a central line in the hospital has changed over time(2). Central line placement was originally a rite of internship with throngs of interns going through a watch one, do one, teach one process.
Today in most institutions, the number of specialties has decreased, and surprisingly, radiology is now the dominant group in many locations, surpassing surgery and anesthesiology as the most common specialty. (2)
Between 1992 and 2011, temporary and long-term CVA placement procedures increased from 638,703 to 808,071 (+27%) and from 76,444 to 316,042 (+313%), respectively.
For temporary central venous catheters, radiology (from 0.4% in 1992 to 32.6% in 2011) now exceeds anesthesiology (from 37% to 22%) and surgery (from 30.4% to 11.7%) as the dominant provider group.
Although volumes remain small (<10% of all procedures), midlevel practitioners have experienced >100-fold growth for most services.
A Comparative Analysis
Let’s compare manometry and ultrasound across key aspects to determine their suitability in different clinical scenarios.
| Aspect | Manometry | Ultrasound |
|---|---|---|
| Safety | Provides pressure readings to confirm venous placement. | Offers superior safety through real-time visualization. |
| Accuracy | Accurate pressure measurements | Provides high accuracy in visualizing veins and structures. |
| Speed | May require an additional 10 – 15 seconds to perform manometry | Typically speeds up the procedure with real-time guidance. |
| Accessibility | Universally accessible | Requires equipment and expertise but increasingly available. |
| Cost | Generally cost-effective using basic IV tubing. | May be more expensive due to equipment and training. |
Clinical Scenarios: Choosing the Right Technique
The choice between manometry and ultrasound should align with the clinical context and individual patient factors. Here are scenarios where one technique may be preferred:
Manometry
- Routine Cases: For straightforward central venous catheterization where the anatomy is clear, manometry provides adequate confirmation.
- Limited Resources: In settings with limited access to ultrasound equipment, manometry remains valuable.
Related Post: Comparing French Sizing to Gauge for IVs and Central Venous Catheters
Ultrasound
- Challenging Anatomy: When dealing with complex anatomy, like obesity or distorted vasculature, ultrasound offers essential visual guidance.
- High-Risk Patients: Patients at high risk of complications benefit from ultrasound’s added safety.
- Complex Procedures: During intricate procedures requiring precise catheter placement, such as hemodialysis access, ultrasound’s real-time visualization shines.
References:
(1) Domino KB, Bowdle TA, Posner KL, Spitellie PH, Lee LA, Cheney FW. Injuries and liability related to central vascular catheters: a closed claims analysis. Anesthesiology. 2004 Jun;100(6):1411-8. doi: 10.1097/00000542-200406000-00013. PMID: 15166560.
(2) Duszak R Jr, Bilal N, Picus D, Hughes DR, Xu BJ. Central venous access: evolving roles of radiology and other specialties nationally over two decades. J Am Coll Radiol. 2013 Aug;10(8):603-12. doi: 10.1016/j.jacr.2013.02.002. Epub 2013 Jun 14. PMID: 23770064.
(3) McGee DC, Gould MK. Preventing complications of central venous catheterization. N Engl J Med. 2003 Mar 20;348(12):1123-33. doi: 10.1056/NEJMra011883. PMID: 12646670.
(4) Bell J, Goyal M, Long S, Kumar A, Friedrich J, Garfinkel J, Chung S, Fitzgibbons S. Anatomic Site-Specific Complication Rates for Central Venous Catheter Insertions. J Intensive Care Med. 2020 Sep;35(9):869-874. doi: 10.1177/0885066618795126. Epub 2018 Sep 19. PMID: 30231668.
(5) Björkander M, Bentzer P, Schött U, Broman ME, Kander T. Mechanical complications of central venous catheter insertions: A retrospective multicenter study of incidence and risks. Acta Anaesthesiol Scand. 2019 Jan;63(1):61-68. doi: 10.1111/aas.13214. Epub 2018 Jul 11. PMID: 29992634.
(6) Sznajder JI, Zveibil FR, Bitterman H, Weiner P, Bursztein S. Central vein catheterization. Failure and complication rates by three percutaneous approaches. Arch Intern Med. 1986 Feb;146(2):259-61. doi: 10.1001/archinte.146.2.259. PMID: 3947185.
(7) Mansfield PF, Hohn DC, Fornage BD, Gregurich MA, Ota DM. Complications and failures of subclavian-vein catheterization. N Engl J Med. 1994 Dec 29;331(26):1735-8. doi: 10.1056/NEJM199412293312602. PMID: 7984193.
(8) Sulek CA, Blas ML, Lobato EB. A randomized study of left versus right internal jugular vein cannulation in adults. J Clin Anesth. 2000 Mar;12(2):142-5. doi: 10.1016/s0952-8180(00)00129-x. PMID: 10818329.
(9)Eisen LA, Narasimhan M, Berger JS, Mayo PH, Rosen MJ, Schneider RF. Mechanical complications of central venous catheters. J Intensive Care Med. 2006 Jan-Feb;21(1):40-6. doi: 10.1177/0885066605280884. PMID: 16698743.
(10) Bowdle A, Kharasch E, Schwid H. Pressure waveform monitoring during central venous catheterization. Anesth Analg. 2009 Dec;109(6):2030-1; author reply 2031. doi: 10.1213/ANE.0b013e3181bea01d. PMID: 19923541.
(11)Ezaru CS, Mangione MP, Oravitz TM, Ibinson JW, Bjerke RJ. Eliminating arterial injury during central venous catheterization using manometry. Anesth Analg. 2009 Jul;109(1):130-4. doi: 10.1213/ane.0b013e31818f87e9. Epub 2009 Apr 17. PMID: 19377052.
(12) Augoustides JG, Horak J, Ochroch AE, Vernick WJ, Gambone AJ, Weiner J, Pinchasik D, Kowalchuk D, Savino JS, Jobes DR. A randomized controlled clinical trial of real-time needle-guided ultrasound for internal jugular venous cannulation in a large university anesthesia department. J Cardiothorac Vasc Anesth. 2005 Jun;19(3):310-5. doi: 10.1053/j.jvca.2005.03.007. PMID: 16130056
(13) Brass P, Hellmich M, Kolodziej L, Schick G, Smith AF. Ultrasound guidance versus anatomical landmarks for internal jugular vein catheterization. Cochrane Database Syst Rev. 2015 Jan 9;1(1):CD006962. doi: 10.1002/14651858.CD006962.pub2. PMID: 25575244; PMCID: PMC6517109.
(14) Gebhard RE, Szmuk P, Pivalizza EG, Melnikov V, Vogt C, Warters RD. The accuracy of electrocardiogram-controlled central line placement. Anesth Analg. 2007 Jan;104(1):65-70. doi: 10.1213/01.ane.0000250224.02440.fe. PMID: 17179244.
(15) Guilbert MC, Elkouri S, Bracco D, Corriveau MM, Beaudoin N, Dubois MJ, Bruneau L, Blair JF. Arterial trauma during central venous catheter insertion: Case series, review and proposed algorithm. J Vasc Surg. 2008 Oct;48(4):918-25; discussion 925. doi: 10.1016/j.jvs.2008.04.046. Epub 2008 Aug 13. PMID: 18703308.
Vascular complications – get surgery involved: